Pain Reprocessing Therapy and
CBT for Pain Management in
Los Angeles and California-wide
Chronic Pain Stole Your Life.
It's Time to Take It Back.
Evidence-based Pain Reprocessing Therapy and Cognitive Behavioral Therapy from doctoral psychologists in Los Angeles.
Structured treatment, measurable progress, and skills you keep for life.
Start Feeling Better This Week.
If you've been living with chronic pain, you've probably been told some version of the same story: the pain is in your body, so the solution must be in your body too. More imaging. More injections. More medication. And yet the pain persists. For many people, this isn't because the treatments failed. It's because the story was incomplete.
Pain Reprocessing Therapy and CBT for pain management offer a fundamentally different starting point. Rather than treating pain as purely a body problem, these evidence-based approaches recognize that your brain plays a central role in generating, amplifying, and maintaining chronic pain. At Cognitive Behavioral Therapy Los Angeles, our doctoral-level psychologists (PsyD/PhD) provide both Pain Reprocessing Therapy (PRT) and cognitive behavioral therapy (CBT) for chronic pain, available in-person at our Los Angeles offices and online across California.
This isn't about dismissing your pain. It's about understanding it more accurately so you can actually do something about it.
What Is Pain Reprocessing Therapy?
Pain Reprocessing Therapy (PRT) is a psychological treatment that helps people with chronic pain by changing their beliefs about the causes and threat value of their pain. PRT teaches patients to reappraise pain signals as non-dangerous brain-generated sensations rather than evidence of tissue damage, which can reduce or eliminate chronic pain. It was developed by psychologist Alan Gordon and validated in a randomized controlled trial published in JAMA Psychiatry.
How Does CBT Help with Chronic Pain?
CBT for chronic pain works by helping people identify and change the attentional processes, thoughts, emotions, and behaviors that amplify pain and keep them stuck in cycles of avoidance and suffering. Through structured skills training, cognitive restructuring, mindfulness strategies, relaxation techniques, and graded behavioral experiments, CBT equips people with practical tools to regain functioning and reduce pain's grip on daily life.
The Puzzle of Chronic Pain: Why It Persists
Here's something that puzzles most people when they first hear it: roughly 85% of chronic back pain cases have no identifiable structural cause. Doctors call this "primary" or "nonspecific" pain. The MRI might show disc changes, but those same changes appear in people who feel perfectly fine.
This creates a frustrating paradox. Your pain is absolutely real. And yet imaging can't explain it. That gap between what the scans show and what you experience is where modern pain science has made its most important discoveries.
Your Brain Has a Volume Knob for Pain
Think of your nervous system like a home alarm system. When you sprain your ankle, pain signals travel from the injury to your brain, and you feel pain. That's the alarm working as designed.
But what happens when the alarm gets stuck? When the brain keeps sending danger signals long after tissues have healed?
Central sensitization occurs when the nervous system becomes chronically over-reactive, amplifying pain signals even in the absence of new tissue damage. The volume knob on pain has been turned up, and it's gotten stuck there. Stress, anxiety, fear about the pain itself, and even just paying close attention to your body can all keep that volume elevated.
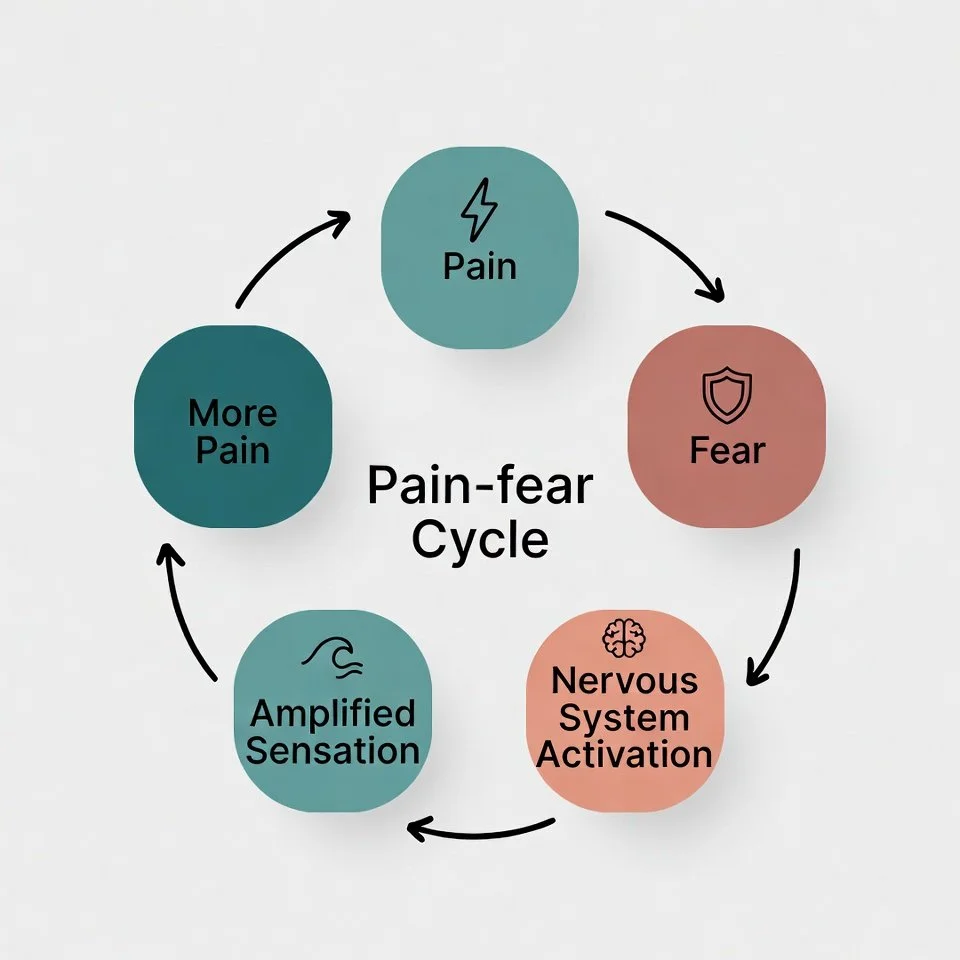
The Pain-Fear Cycle
The pain-fear cycle is a self-reinforcing loop in which pain triggers fear, fear heightens the nervous system's sensitivity, and that sensitivity generates more pain.
Pain shows up. You feel afraid, because pain usually means something is wrong. That fear puts your nervous system on higher alert. Ordinary sensations get interpreted as threatening. More pain follows, which creates more fear, and the cycle tightens.
This isn't a character flaw or a sign of weakness. It's your brain doing exactly what evolution designed it to do: protect you from perceived danger. The problem is that the danger assessment is wrong.
How Chronic Pain Shows Up in Real Life
Activities and Avoidance
You stop doing things you used to enjoy. Maybe you skip social events because you're worried about a flare-up. Maybe you've given up exercise, hobbies, even career goals. The logic feels airtight: if movement causes pain, stop moving. But reduced activity leads to deconditioning, which makes your body more sensitive, which creates more pain.
Thoughts and Emotions
On bad pain days, your thinking shifts. "This is never going to get better." "I can't handle this." These thoughts feel like observations, but they function more like accelerants. Negative thoughts open the gate to more pain. Depression, anxiety, and helplessness follow, and each dials up the nervous system's threat response. Chronic pain often travels with these conditions, and treating them together matters.
The Overwork-Crash Pattern
Many high-functioning people with chronic pain develop a specific pattern. On a good day, you push through everything on your list. Then you spend the next two days recovering from a flare-up, and push again to make up for lost time. This boom-and-bust cycle keeps pain unpredictable and life exhausting.
If you recognize yourself in any of these patterns, you're not alone, and there are structured, evidence-based ways to change them. If you'd like to explore whether this approach might fit, we offer a free 15-minute consultation to help you decide.
How PRT and CBT Work Together to Treat Chronic Pain
At our practice, we don't treat PRT and CBT as competing philosophies. Because our clinicians are trained in both, your treatment plan is matched to your assessment rather than limited to a single approach. If centralized pain is the primary driver, your therapist can lead with PRT. If behavioral and emotional factors are prominent, CBT skills take the lead. For many people, elements of both are woven together.
Pain Reprocessing Therapy: Changing Your Brain's Interpretation
PRT starts with a powerful reframe: for many people, chronic pain is like a false alarm. The alarm is genuinely going off, but there's no fire. The pain is real, and your body isn't damaged.
Education and evidence gathering. Your therapist helps you compile personalized evidence that your pain is centrally driven rather than structural. Maybe your pain started during a stressful period, moves around your body, or is worse at work and barely there on vacation. Each piece of evidence helps shift your understanding.
Somatic tracking. Somatic tracking is a technique in which you observe pain sensations with mindful curiosity while your therapist reinforces messages of safety, gradually retraining your brain's threat response. Instead of bracing against pain or trying to ignore it, you learn to notice the sensation without trying to change it. Over time, this rewires the brain's danger assessment.
Addressing emotional threats. PRT also reduces your overall threat level. Unprocessed emotions, self-criticism, perfectionism, and chronic stress keep the nervous system on high alert. As these patterns are addressed, the brain becomes less likely to interpret ordinary body signals as dangerous.
Does Pain Reprocessing Therapy Work?
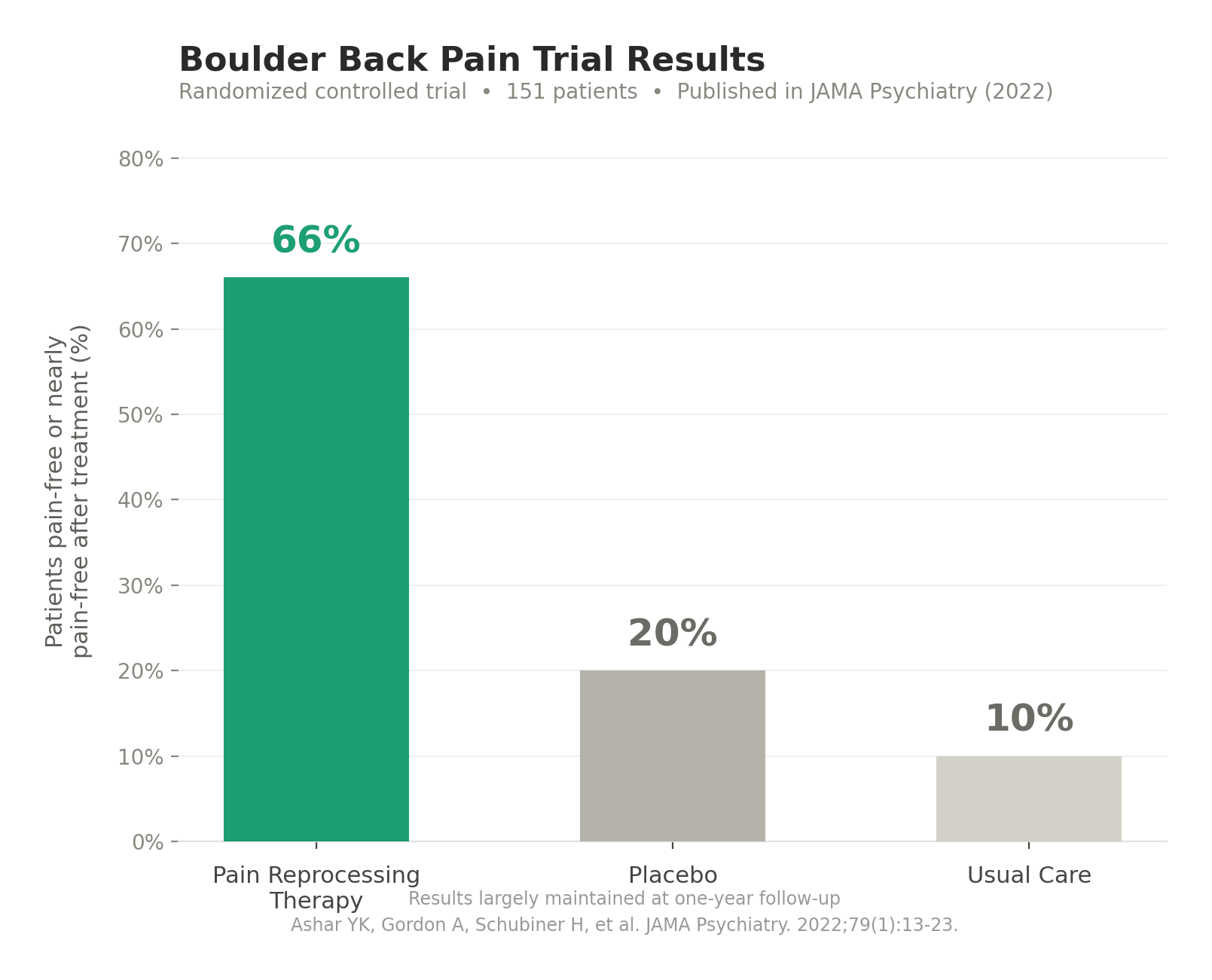
The evidence is striking. In the Boulder Back Pain Trial, 66% of patients who received PRT were pain-free or nearly pain-free after treatment, compared to 10% for those receiving usual care. Results were largely maintained at one-year follow-up. Published in JAMA Psychiatry, the study provided some of the strongest evidence to date that psychological treatment can produce lasting chronic pain relief.
CBT for Pain Management: Building Skills That Last
CBT for chronic pain takes a structured, skills-based approach across roughly 11 to 16 sessions. You learn cognitive restructuring to catch and evaluate the automatic thoughts that amplify pain. You practice relaxation techniques like diaphragmatic breathing and progressive muscle relaxation to reduce the physiological arousal that worsens pain. Time-based activity pacing breaks the overwork-crash cycle by scheduling breaks before pain escalates, so you actually accomplish more across a week. And pleasant activity scheduling deliberately reintroduces enjoyable activities to interrupt the withdrawal and isolation that feed the pain cycle.
If what you've read so far resonates, you don't need to figure out the right approach before reaching out. That's what the assessment is for. You can schedule a free 15-minute consultation or book a full intake directly.
Pain Reprocessing Therapy vs. CBT for Pain: How Are They Different?
PRT aims to eliminate or significantly reduce pain by retraining the brain's threat response, whereas CBT focuses on building coping skills so pain has less control over your life. PRT is best suited for primary or centralized pain without a clear structural cause, while CBT has a broader evidence base spanning back pain, headaches, fibromyalgia, and other conditions.
| Pain Reprocessing Therapy (PRT) | CBT for Pain Management | |
|---|---|---|
| Primary goal | Reduce or eliminate pain by retraining the brain | Improve functioning and coping; reduce pain's impact |
| Core premise | Pain is a reversible, brain-generated false alarm | Thoughts, emotions, and behaviors amplify pain |
| Key techniques | Somatic tracking, safety reappraisal, evidence gathering | Cognitive restructuring, relaxation training, activity pacing |
| Best suited for | Primary/centralized pain without clear structural cause | Pain with significant behavioral and emotional components |
| Typical duration | 8 to 12 sessions | 11 to 16 sessions |
| Evidence base | Randomized controlled trial in JAMA Psychiatry (2021) | Decades of research across multiple pain conditions |
In clinical practice, elements of both are often integrated based on what each person needs.
What Therapy Looks Like at Our Practice
Here's what you can expect if you begin treatment for chronic pain at Cognitive Behavioral Therapy Los Angeles.
The First Few Sessions
Your therapist starts with a thorough assessment: your pain history, what you've already tried, how pain affects your daily life, and your goals. You'll complete brief validated questionnaires that establish a clear baseline. Together, you'll map out the specific factors maintaining your pain.
The Middle Phase
Weekly 50-minute sessions are structured around learning and practicing skills. Your therapist introduces techniques tailored to your situation: somatic tracking, cognitive restructuring, pacing strategies, or some combination. You'll practice between sessions for roughly 10 minutes a day.
Around weeks four through six, you and your therapist review your progress using the same measures from your baseline. This isn't guesswork. You'll see your own data. If something needs adjusting, you adjust it.
The Final Sessions
Treatment is designed to end. The final sessions focus on consolidating skills, planning for pain flare-ups, and ensuring you have a clear strategy for maintaining gains independently.
Clients commonly report returning to activities they'd given up, sleeping better, and relying less on medication. The goal isn't just managing pain. It's reclaiming the parts of your life that pain took away.
Sessions are available in-person at our Brentwood or Pasadena offices and online throughout California.
Addressing the Fears That Keep People from Starting
"What if my pain isn't bad enough to need therapy?"
There's no minimum pain score required. If pain is limiting your activities, affecting your mood, or occupying more mental bandwidth than you'd like, that's enough. Many of the people we see are still functioning at a high level on the outside while struggling considerably on the inside.
"My pain is physical. How can a psychological treatment help?"
This is the most common and most understandable concern. "Psychological" doesn't mean "imaginary." Your pain is generated by your nervous system, which is precisely why psychological approaches can change it. Targeting the brain's pain-processing networks means targeting the actual source of the problem for many chronic pain conditions.
"What if it doesn't work for me?"
The evidence for both PRT and CBT for chronic pain is strong, and we use measurement-based care to track your progress objectively. If you're not seeing movement within the first several weeks, we talk about it openly and adjust.
"I'm worried about the cost."
We're out-of-network, and we provide superbills that many PPO plans reimburse at 50 to 80%. HSA and FSA are accepted. Treatment is structured and time-limited, typically 11 to 16 sessions. The skills you learn are yours to keep.
Frequently Asked Questions
What is Pain Reprocessing Therapy (PRT)? Pain Reprocessing Therapy is an evidence-based treatment that helps people with chronic pain by retraining the brain to interpret body signals as safe rather than dangerous. It uses techniques including somatic tracking, safety reappraisal, and evidence gathering. PRT was validated in a randomized controlled trial showing significant and lasting pain relief.
How is CBT for chronic pain different from regular talk therapy? CBT for chronic pain is structured, goal-directed, and skills-based. Each session teaches specific techniques like cognitive restructuring, relaxation training, and activity pacing. Your therapist tracks your progress with validated measures. It's designed to create measurable change in a defined timeframe, not to provide open-ended emotional support.
Can PRT and CBT be combined in the same treatment? Yes. Many clinicians integrate elements of both approaches based on the individual assessment. PRT focuses on reappraising pain as non-dangerous, while CBT builds practical coping skills and addresses behavioral patterns. The combination can be particularly effective for people with both centralized pain and significant activity avoidance.
How long does treatment typically take? PRT typically involves 8 to 12 sessions and CBT for chronic pain involves 11 to 16 sessions. Treatment length depends on pain complexity, treatment goals, and how quickly skills are acquired. Your therapist reviews progress around sessions four through six and adjusts the plan accordingly.
What types of chronic pain respond to PRT and CBT? Both approaches have evidence for back pain, headaches, fibromyalgia, and other conditions. PRT is particularly suited for centralized pain where no clear structural cause has been identified. CBT has a broader evidence base spanning many pain conditions. A thorough assessment helps determine the best fit.
Can I do PRT or CBT for pain management online? Yes. Both approaches can be delivered effectively through telehealth. Our practice offers online sessions to clients throughout California. Research supports that telehealth-delivered psychological pain treatments produce comparable outcomes to in-person treatment.
What if I'm already taking pain medication? You don't need to stop medication to begin PRT or CBT. Many people find that as they develop new pain management skills, they're able to gradually reduce their reliance on medication in consultation with their prescribing physician. Medication changes should always be guided by your medical provider.
How do I know if my pain is "centralized" versus structural? Several indicators suggest centralized pain: pain that started during a stressful period, pain that moves locations, inconsistency between imaging findings and symptoms, pain that varies with mood or stress, and the presence of multiple pain-related conditions. Your therapist can help you evaluate these factors during the assessment.
Taking the First Step
Pain Reprocessing Therapy and CBT for chronic pain are about understanding the actual mechanisms that keep pain going and developing the skills to change them.
At Cognitive Behavioral Therapy Los Angeles, our doctoral-level psychologists specialize in evidence-based chronic pain treatment. Schedule a free 15-minute phone consultation or book an intake appointment directly.
You can reach us at (310) 254-9748. We see clients in-person at our Westwood and Pasadena offices and online across California.
Clinically reviewed by Albert Bonfil, PsyD. Last updated March 2026.